The coronavirus pandemic will have huge impacts on the National Health Service (NHS). Patients suffering from the illness are placing unprecedented demands on acute care, particularly on intensive care units (ICUs). This has led to an effort to dramatically increase the resources available to NHS hospitals in treating these patients, involving reorganisation of hospital facilities, redeployment of existing staff and a drive to bring in recently retired and newly graduated staff to fight the pandemic.
These increases in demand and changes to supply will not only affect patients with the coronavirus, but will have large knock-on effects on the care provided to the wider population. Here we discuss likely implications for healthcare delivery in the short and medium term of the responses to the coronavirus pandemic, focusing primarily on the implications for non-coronavirus patients. We first set out the amount of planned and unplanned hospital care that we might expect to take place in the absence of the pandemic and describe how this activity varies across age, socio-economic status and place. We then discuss how the amount and quality of care could be affected. To do this, we draw primarily on past data on NHS activity in England to understand who is most likely to be affected by these changes and evidence from previous research on the impacts of sudden changes in the demand for, and supply of, healthcare. Our analysis, though speculative due to lack of real-time data, suggests that disruptions to non-coronavirus care are likely to have most impact on older and less affluent individuals.
Dealing with coronavirus patients against a backdrop of shortage
The immediate impact of the coronavirus on the NHS is a huge increase in the demand for acute care and, in particular, intensive care facilities. International evidence suggests that the virus affects some groups of the population more severely than others: the death rate is much higher among individuals aged 70 and above than it is among younger individuals, and it is higher among men than among women. Comparable data for the UK are not currently available, and it is not possible to say with precision who is receiving treatment for the coronavirus in NHS intensive care facilities.
What is clear, however, is that meeting the demand for care from coronavirus patients is already stretching hospitals to capacity. There are concerted efforts to boost that capacity, but this is against a backdrop of relatively few spare ICU beds and existing staff shortages.
Historically, the number of ICU beds in the UK has been low by international standards (Rhodes et al., 2012). The number of beds has increased in recent years, but occupancy remains high, with 83% of the 4,123 adult critical care beds in England occupied in January 2020 (NHS England, 2020a). The UK also has low levels of staff compared with other EU countries. For example, in 2015, the UK had fewer doctors for its population size than other European countries, at 2.8 doctors per 1,000 people compared with an EU15 average of 3.9 (Lee and Stoye, 2018). While the total number of doctors and nurses has increased in the last decade, this has been outstripped by the increase in activity. Between 2010 and 2016, the number of full-time-equivalent (FTE) doctors rose by just under 10%, and nurses by around 1%, compared with increases of around 17% in the number of inpatient admissions and an almost 25% increase in the number of outpatient appointments (Lee, Propper and Stoye, 2020). Nursing vacancies were almost 44,000 in England in the first quarter of 2019/20, a figure equivalent to around 12% of the nursing workforce (Gershlick and Charlesworth, 2019).
The effect on care volumes: cancellations, delays and disrupted treatment
To deal with coronavirus cases, the amount of resources available for non-coronavirus patients has already been reduced, though there are no real-time publicly available data available to be able to precisely quantify by how much and for whom.
NHS England has announced its intention to free up around 30,000 of its 100,000 general and acute hospital beds. Around half of this is to be achieved through urgent discharge of patients who are medically fit to leave. The remaining half will come through the postponement of all non-urgent elective operations. This will include procedures such as cataract surgery, joint replacements and gall-bladder removal. In the first three months of 2018, in the midst of a worse-than-usual flu season, 25,502 elective operations were cancelled in England (NHS England, 2020b). The scale of the current pandemic means that the number of cancelled or delayed procedures is likely to be considerably higher this time around, with the number of affected patients potentially running into the hundreds of thousands.
In addition to hospitals delaying or cancelling treatment, it is likely that some patients will postpone or decide against seeking treatment in an attempt to avoid visiting a hospital (potentially storing up health problems for the future). There are signs of this in emergency care: the number of accident and emergency (A&E) attendances has fallen by almost half since the beginning of March (possibly due to self-isolation and/or the decrease in traffic, pollution and workplace accidents following the current fall in economic activity). Nonetheless, as shown below, emergency admissions usually make up around half of admissions to hospitals and there will be ongoing requirements for (non-coronavirus-related) emergency care.
We can use data on past NHS activity in England to examine who is likely to be affected by changes to their care, either due to cancellations or delays to elective treatment or due to reductions in emergency care. The immediate effects of the pandemic are currently projected to be highest between April and June this year. We use data from hospital records that cover this same period from a past year (2017) to examine which groups are mostly likely to be affected by potential disruptions to elective and non-coronavirus emergency care. If disruptions persist for longer than this three-month period then the affected number of patients will be even larger.
Between April and June 2017, a total of 1.7 million patients were admitted for 2.5 million elective procedures (both ‘urgent’ and ‘non-urgent’) across England. In addition, 1.2 million patients were admitted to NHS hospitals a total of 1.5 million times for emergency (unplanned) reasons over the same period. And while these latter numbers may fall this year through reduced attendances at A&E, a large number of emergency cases will still need to be treated.
Figure 1 shows there is considerable regional variation in both the level of admissions and the split between emergency and elective procedures. As the NHS delays or cancels non-urgent elective procedures, regions in which elective care represents a greater share of hospital activity (London, the North West and the South West) may be better placed to substitute resources towards tackling the coronavirus, although the extent to which elective resources can be used to treat emergency patients effectively remains uncertain.
Figure 1: Total number of NHS elective and emergency admissions between April and June 2017, and coronavirus cases as of 5 April 2020, by English region
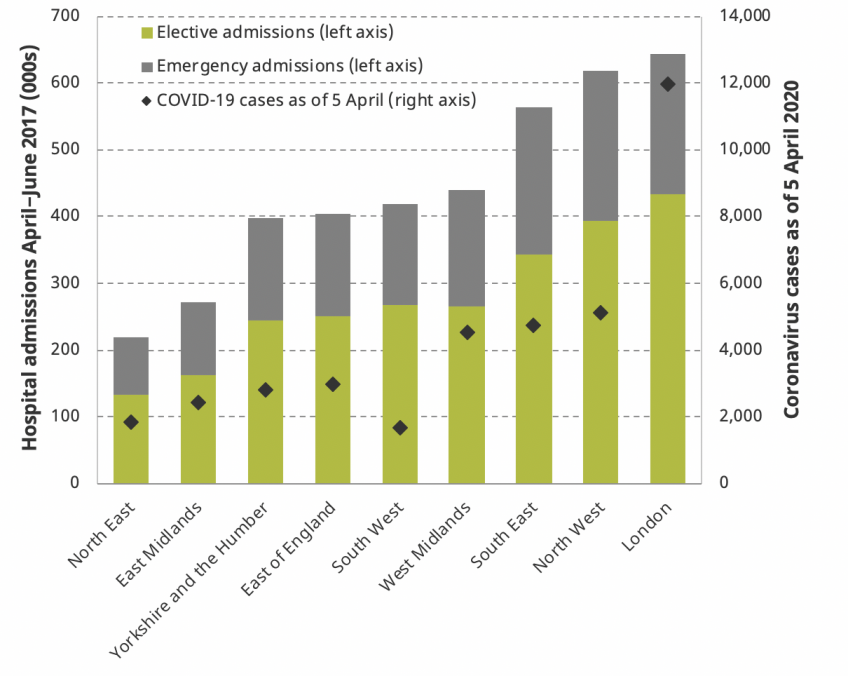
Source: Authors’ calculations using Hospital Episode Statistics 2017 and HM Government, ‘Track coronavirus cases’ (accessed 6 April 2020), https://www.gov.uk/government/publications/covid-19-track-coronavirus-cases.
The effect of the coronavirus outbreak to date has also differed across regions. At the time of writing, the number of cases in London far exceeds the number in any other region. If the differences persist, regions will differ both in how many coronavirus cases they have to deal with and in their capacity to redeploy existing resources towards treating those patients.
It is also clear that the knock-on effects of increased demand for coronavirus care will have larger impacts on some age groups than others. Figure 2 shows the age distribution of NHS hospital admissions in England for April–June 2017. Emergency admissions are highest among children under the age of 10 (with 171,000 admissions over a three-month period) and among those in their 70s and 80s. This pattern in part reflects the number of people in each age group. Figure 3 instead shows the number of admissions over the same April–June period per 1,000 people. The rate of emergency admissions is highest among the population aged 90 and above: 164 emergency admissions for every 1,000 people, versus 27 for the population as a whole. The very oldest in the population are therefore the most likely to have emergency care disrupted in the coming months.
Figure 2: Number of elective and emergency admissions between April and June 2017, by ten-year age group
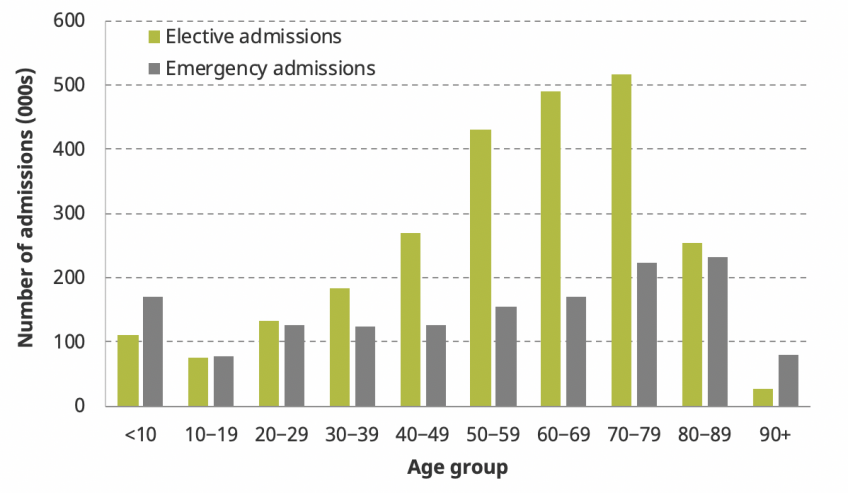
Note and source: Authors’ calculations using the Hospital Episode Statistics (HES) Admitted Patient Care data set. Includes all NHS-funded patients treated in England between 1 April and 30 June 2017. Elective patients are those with pre-planned admissions. Emergency patients are others, excluding maternity and delivery admissions.
Figure 3: Rates of elective and emergency admissions between April and June 2017, by ten-year age group
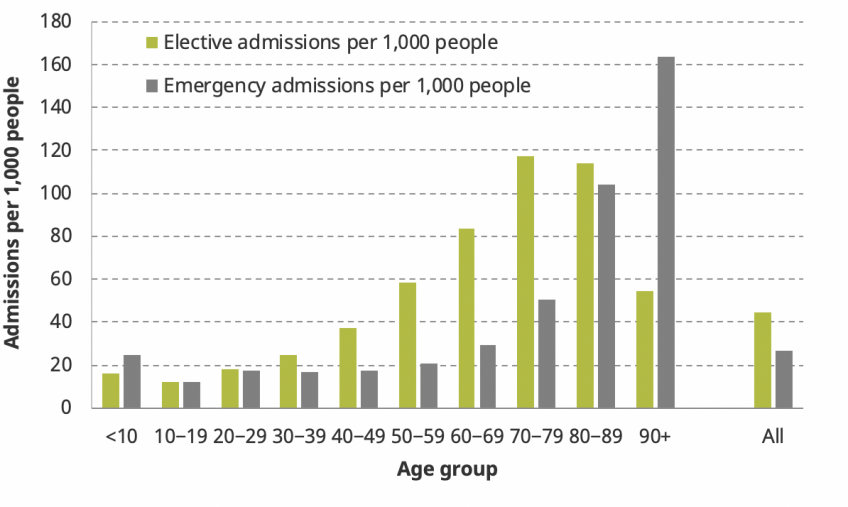
Note and source: Authors’ calculations using the Hospital Episode Statistics (HES) Admitted Patient Care data set and ONS population estimates. Includes all NHS-funded patients treated in England between 1 April and 30 June 2017. Elective patients are those with pre-planned admissions. Emergency patients are others, excluding maternity and delivery admissions.
Figure 4: Number of elective and emergency admissions between April and June 2017, by local area deprivation
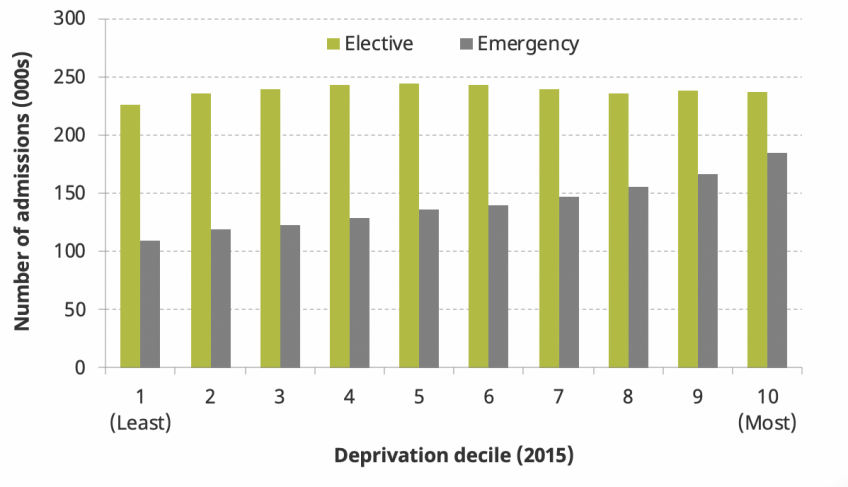
Note and source: Authors’ calculations using the Hospital Episode Statistics (HES) Admitted Patient Care data set. Includes all NHS-funded patients treated in England between 1 April and 30 June 2017. Elective patients are those with pre-planned admissions. Emergency patients are others, excluding maternity and delivery admissions. Deprivation deciles are defined using the ONS 2015 Index of Multiple of Deprivation series. Deprivation increases with decile number (10 = most deprived 10% of areas).
Older people are heavier users of elective hospital care than younger people. There were 517,000 elective admissions for people in their 70s compared with only 184,000 admissions for people in their 30s, despite the fact that there are 3 million more people in the younger age group living in England. Put another way, there were 117 and 114 elective admissions per 1,000 people for those in their 70s and 80s, respectively, but just 25 for every 1,000 people in their 30s. This means that the burden of delays to elective care is also most likely to fall on the older population (although rates of use of elective care are lower for the very oldest individuals, aged 90 and above).
It is also likely that the impact will not be evenly felt across individuals of different socio-economic status. Figure 4 shows the number of elective and emergency NHS hospital admissions in England between April and June 2017 across areas ranked by (lowest to highest) deprivation (as measured by the deprivation of the small area (LSOA) where the patient lives). Approximately a tenth of the population live in each decile so the figures can also be interpreted as rates.
Elective admissions are relatively evenly distributed across patients from differently deprived areas, with between 225,000 and 250,000 admissions in each group during the period. By contrast, the number of emergency admissions is clearly higher among more deprived areas than in less deprived areas. In particular, there were 185,194 emergency admissions among residents living in the most 10% deprived areas of the country over the three-month period, in comparison with only 108,948 in the least 10% deprived areas.
Taken together, this suggests that potential disruptions to emergency care will disproportionately impact older people and those who are the least affluent.
There may also be knock-on effects on the NHS from disruptions to the social care workforce and subsequent reductions in the amount or quality of social care provided. Around 1.5 million people work in the adult social care sector in England. These workers will be subject to similar risks to those facing many workers within the NHS, and we might expect similarly high rates of absence due to the coronavirus. Staffing shortages could lead to an increase in the number of older people not receiving care that adequately meets their needs and possibly also more pressure on A&E departments. Crawford, Stoye and Zaranko (2018) showed that sharp reductions in the number of older people receiving publicly funded social care in their own home (the results of cuts to local authority spending on social care in the years after 2010) were accompanied by an increase in the number of visits to A&E by people aged 65 and above. Again, the group who will be most affected are those who are older.
The effect on care quality
Despite huge increases in staff who have come out of retirement or joined the workforce early (for example, the Royal College of Nursing (RCN) estimates that 7,000 recently retired nurses have returned, and final-year nursing students are doing clinical placements, adding perhaps another 3,000 nurses), there will be fewer staff available for treating other patients as more staff focus on treating coronavirus patients. This will be exacerbated by the effects of the virus itself on staff numbers, with recent estimates from the Royal College of Physicians and the RCN suggesting that up to a quarter of NHS doctors and nurses have had to take time off already because of sickness or self-isolation. Furthermore, staff are likely to be working in unfamiliar settings. This raises the question of what is likely to happen to the outcomes of non-patients if they are treated by fewer, or by different, staff than usual.
We know from existing work that the reduced availability of hospital staff – due to either illness or being reassigned elsewhere – is likely to have negative effects on quality of care and on patient outcomes. Gruber and Kleiner (2012) show that reductions in the numbers of nursing staff present in hospitals during nursing strikes in the US led to an increase in mortality and readmissions among patients, even after adjusting for changes in demographics and case mix in these hospitals. Needleman et al. (2011) show that hospital shifts with nurse staffing levels below the target level are associated with increased levels of mortality. Friedrich and Hackmann (2017) show that a reduction in nursing employment in Denmark had detrimental effects on the quality of care provided by hospitals.
Even if numbers can be shored up, the composition and experience of the team, as well as its size, matter for the care that is provided to patients. Bartel et al. (2014) show, in a US context, that when nursing teams were disrupted by the departure of an experienced member or the arrival of a new hire, team productivity fell and patient outcomes suffered as a result. Chan (2020) shows that experience matters for doctor decision-making and resultant patient outcomes.
It is difficult to draw firm conclusions about the likely scale of the impact on patient outcomes from coronavirus-related staffing disruptions, in part because the scale of those disruptions is not yet clear. But Gruber and Kleiner (2012), for example, show that in-hospital mortality was almost 20% higher for patients admitted during a nursing strike (the typical length of which was 19 days). The coronavirus outbreak will likely lead to similar levels of disruption to nursing teams in the months to come, given that nurses displaying symptoms will be unable to work for an extended period. Doctors and other healthcare workers will be similarly affected. We would therefore expect similar, and quite possibly even larger, adverse effects on patient outcomes.
In sum, given that NHS care is focused upon older and more deprived individuals, it is likely that those who will bear the highest costs of coronavirus are this population, both now and in the medium term. This is only likely to exacerbate existing inequalities in health across place and socio-economic status.
Longer-term concerns
Finally, we consider two longer-term impacts, both of which have implications for the public purse. First, it is clear that staffing issues will loom large. While staff have come out of retirement to deal with the immediate crisis, after it is over they will presumably return to retirement. In addition, if staff cannot be protected against the virus, it may reduce the attractiveness of work in the NHS in the future. And the worldwide nature of the pandemic may mean that the NHS’s ability to recruit from overseas may well fall (and this is in addition to any pressures from leaving the European Union). The Conservatives’ 2019 general election manifesto already pledged to find an additional 50,000 nurses by 2024–25. The impact of the coronavirus may mean they need to find more. With many areas already experiencing nursing shortages, it is hard to see how this can be achieved without an increase in nurses’ wages in shortage areas. This in turn would push up the cost of the NHS for taxpayers.
Second, waiting times for elective care will rise. Whilst waiting times are still well below their levels in the early 1990s and before, they have been rising recently, causing public concern. The response to the coronavirus will only increase the length of waits. Historically, increased waiting times in the NHS have led to an increased demand for private care (Besley, Hall and Preston, 1999). While incomes and employment are currently hard hit by the social isolation measures that have been imposed, these measures are not likely to affect the incomes of all equally. For example, recent research at IFS shows that low earners are seven times as likely as high earners to have worked in a sector that is now shut down (Joyce and Xu, 2020). Some better-off individuals may respond to rising waiting times and staff shortages by purchasing private care, thus exacerbating existing inequalities in receipt of healthcare. But these individuals would remain reliant on the NHS for – among other things – emergency care. There has been a recent groundswell in support for the NHS, and satisfaction with the health service had already risen prior to the coronavirus pandemic. In the coming years, this may translate into greater support for tax rises to fund higher levels of health spending. Whatever the outcome, it is clear that the current crisis will mean that choices about how much to fund the NHS and how to spend those funds will be an even more central part of the political agenda.